UKMLA AKT FREE TRIAL
The best and most comprehensive resources customised for success in the UKMLA AKT Exam.
No sign-up required.
Comprehensive Resources
Explore our range of topics
Topics are aligned based on the MLA Content Map
-
✅Acute and emergency
-
✅Allergy and immunology
-
✅Cardiovascular
-
✅Child health
-
✅Haematology
-
✅Pharmacology and therapeutics
-
✅Dermatology
-
✅Ear, nose and throat
-
✅Endocrine and metabolic
-
✅Respiratory
-
✅Infectious diseases
-
✅Medical ethics and law
-
✅Mental health
-
✅Musculoskeletal
-
✅Ophthalmology
-
✅Palliative and end of life care
-
✅Rheumatology
-
✅Surgery
-
✅Perioperative medicine, Anaesthetics
-
✅Genitourinary, Cancer
-
✅General practice and primary healthcare
-
✅Anatomy & Genetics
-
✅Neurosciences
-
✅Obstetrics and gynaecology
-
✅Sexual Health
-
✅Renal and urology
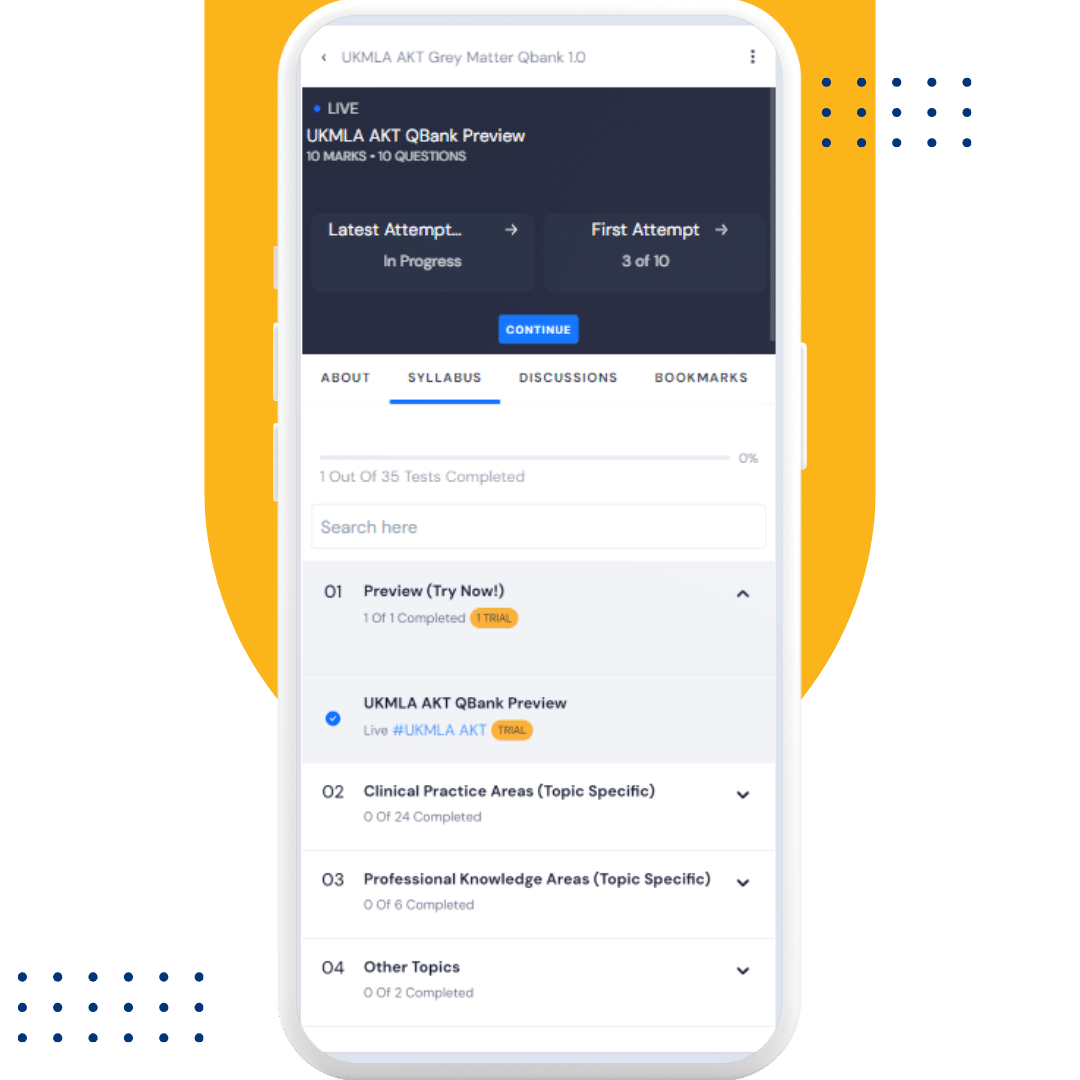
UKMLA AKT QBank
UKMLA AKT Free Trial
Quiz-summary
0 of 10 questions completed
Questions:
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
Information
Give our UKMLA AKT questions a try for free!
Our questions are designed to match the content outlined in the GMC MLA Content Map, ensuring that our QBank aligns perfectly with the exam material. We’re confident that using our QBank will significantly improve your chances of passing the exam.
You have already completed the quiz before. Hence you can not start it again.
Quiz is loading...
You must sign in or sign up to start the quiz.
You have to finish following quiz, to start this quiz:
Results
0 of 10 questions answered correctly
Your time:
Time has elapsed
You have reached 0 of 0 points, (0)
Categories
- Acute and emergency 0%
- Allergy and immunology 0%
- Cancer 0%
- Cardiovascular 0%
- Child health 0%
- Clinical haematology 0%
- Dermatology 0%
- Endocrine and metabolic 0%
- ENT 0%
- Pharmacology and therapeutics 0%
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- Answered
- Review
-
Question 1 of 10
1. Question
A 28-year-old man with a history of epilepsy is brought to the emergency department (ED) by ambulance after being found unconscious. The ambulance crew reports that he was having a seizure when they arrived. The patient is now awake but confused and has a Glasgow Coma Scale (GCS) of 13. He smells of alcohol. His blood pressure is 160/93 mmHg and temperature is 37.9°C. On examination, there is a quiet systolic murmur.
Which of the following investigations is most useful at this stage?
Correct
The patient is a known epileptic and has just had a seizure. The most likely cause of the seizure is a seizure disorder, but it is important to check his phenytoin levels to make sure that he is taking the correct dose of medication. If his phenytoin levels are low, then he may need to be given more medication.
The other options are less likely to be helpful at this stage.
- A CT scan of the brain can be used to rule out other causes of seizures, such as a head injury or stroke, but it is not necessary in this case because the patient has a history of epilepsy.
- An EEG can be used to diagnose seizure disorders, but it is not as good as phenytoin levels for checking medication compliance.
- An echocardiogram can be used to look for heart problems, but it is not likely to be helpful in this case.
- An MRI of the brain can be used to look for more subtle abnormalities than a CT scan, but it is not usually necessary in the acute setting.
Incorrect
The patient is a known epileptic and has just had a seizure. The most likely cause of the seizure is a seizure disorder, but it is important to check his phenytoin levels to make sure that he is taking the correct dose of medication. If his phenytoin levels are low, then he may need to be given more medication.
The other options are less likely to be helpful at this stage.
- A CT scan of the brain can be used to rule out other causes of seizures, such as a head injury or stroke, but it is not necessary in this case because the patient has a history of epilepsy.
- An EEG can be used to diagnose seizure disorders, but it is not as good as phenytoin levels for checking medication compliance.
- An echocardiogram can be used to look for heart problems, but it is not likely to be helpful in this case.
- An MRI of the brain can be used to look for more subtle abnormalities than a CT scan, but it is not usually necessary in the acute setting.
-
Question 2 of 10
2. Question
A 12-year-old girl is brought to the emergency department 3 hours after the sudden onset of colicky abdominal pain and vomiting. She also has redness and swelling of the face and lips without pruritus. Her symptoms began following a tooth extraction earlier this morning. She had a similar episode of facial swelling after a bicycle accident 1 year ago which resolved within 48 hours without treatment. Vital signs are within normal limits. Examination shows a nontender facial edema, erythema of the oral mucosa, and an enlarged tongue. The abdomen is soft, and there is tenderness to palpation over the lower quadrants. An abdominal ultrasound shows segmental thickening of the intestinal wall.
Which of the following is the most likely cause of this patient’s condition?
Correct
Complement inhibitor deficiency or, more specifically, C1 inhibitor deficiency, is the underlying cause of hereditary angioedema. A deficiency or dysfunction of C1 inhibitor results in elevated levels of bradykinin, which is as a strong vasodilator. Hereditary angioedema is characterized by recurrent episodes of swelling without urticaria or pruritus that primarily affects the skin and mucosa of the gastrointestinal and upper respiratory tracts. The most common triggers are stress and trauma, especially from dental procedures. The episodes are usually self-limiting and resolve within 2–4 days, as was the case in this patient’s previous attack. Hereditary angioedema is an autosomal dominant disorder. However, about 25% of cases are due to spontaneous mutations.
Incorrect Answers:
- Drug-induced bradykinin excess: While bradykinin excess is involved in HAE, it is not typically caused by drug-induced mechanisms. HAE is a genetic disorder.
- Autoantibody-mediated tissue damage: HAE is not caused by autoantibodies, but rather by a deficiency in C1-INH.
- Immune-complex deposition: Immune-complex deposition is associated with conditions like immune complex glomerulonephritis, but it is not the cause of this patient’s symptoms.
- Leukotriene overproduction: Leukotriene overproduction is associated with conditions like asthma and allergic reactions, but it is not the cause of the symptoms described in this patient, which are more indicative of HAE.
Incorrect
Complement inhibitor deficiency or, more specifically, C1 inhibitor deficiency, is the underlying cause of hereditary angioedema. A deficiency or dysfunction of C1 inhibitor results in elevated levels of bradykinin, which is as a strong vasodilator. Hereditary angioedema is characterized by recurrent episodes of swelling without urticaria or pruritus that primarily affects the skin and mucosa of the gastrointestinal and upper respiratory tracts. The most common triggers are stress and trauma, especially from dental procedures. The episodes are usually self-limiting and resolve within 2–4 days, as was the case in this patient’s previous attack. Hereditary angioedema is an autosomal dominant disorder. However, about 25% of cases are due to spontaneous mutations.
Incorrect Answers:
- Drug-induced bradykinin excess: While bradykinin excess is involved in HAE, it is not typically caused by drug-induced mechanisms. HAE is a genetic disorder.
- Autoantibody-mediated tissue damage: HAE is not caused by autoantibodies, but rather by a deficiency in C1-INH.
- Immune-complex deposition: Immune-complex deposition is associated with conditions like immune complex glomerulonephritis, but it is not the cause of this patient’s symptoms.
- Leukotriene overproduction: Leukotriene overproduction is associated with conditions like asthma and allergic reactions, but it is not the cause of the symptoms described in this patient, which are more indicative of HAE.
-
Question 3 of 10
3. Question
A 6-year-old boy presents with a 1-month history of aching bones and muscle pains. On examination, he appears pale, has multiple bruises on his legs, and extensive lymphadenopathy is noted. Blood tests reveal the presence of blast cells on the blood film. What is the most likely diagnosis?
Correct
The clinical presentation of a 6-year-old with aching bones, muscle pains, pallor, multiple bruises, lymphadenopathy, and blast cells on the blood film strongly suggests acute lymphoblastic leukemia (ALL). ALL is a common pediatric malignancy characterized by the overproduction of immature lymphoblasts. This condition typically presents with nonspecific symptoms such as bone pain, fatigue, and bruising due to bone marrow infiltration by leukemic cells.
Incorrect Answers:
- Child abuse: Child abuse does not typically manifest with the hematological findings described in the case, such as blast cells in the blood film. This option is not supported by the clinical presentation.
- Henoch–Schönlein purpura: Henoch–Schönlein purpura is a vasculitis that primarily affects small blood vessels and is characterized by purpura, abdominal pain, joint pain, and renal involvement. It does not usually present with the extensive lymphadenopathy and blast cells seen in this case.
- Juvenile idiopathic arthritis: Juvenile idiopathic arthritis is a chronic inflammatory condition that primarily affects the joints. It does not typically cause extensive lymphadenopathy or blast cells in the blood, making it an unlikely diagnosis in this case.
- Sickle cell disease: Sickle cell disease primarily presents with symptoms related to vaso-occlusive crises, anemia, and hemolysis. It does not typically involve extensive lymphadenopathy or blast cells in the blood.
Incorrect
The clinical presentation of a 6-year-old with aching bones, muscle pains, pallor, multiple bruises, lymphadenopathy, and blast cells on the blood film strongly suggests acute lymphoblastic leukemia (ALL). ALL is a common pediatric malignancy characterized by the overproduction of immature lymphoblasts. This condition typically presents with nonspecific symptoms such as bone pain, fatigue, and bruising due to bone marrow infiltration by leukemic cells.
Incorrect Answers:
- Child abuse: Child abuse does not typically manifest with the hematological findings described in the case, such as blast cells in the blood film. This option is not supported by the clinical presentation.
- Henoch–Schönlein purpura: Henoch–Schönlein purpura is a vasculitis that primarily affects small blood vessels and is characterized by purpura, abdominal pain, joint pain, and renal involvement. It does not usually present with the extensive lymphadenopathy and blast cells seen in this case.
- Juvenile idiopathic arthritis: Juvenile idiopathic arthritis is a chronic inflammatory condition that primarily affects the joints. It does not typically cause extensive lymphadenopathy or blast cells in the blood, making it an unlikely diagnosis in this case.
- Sickle cell disease: Sickle cell disease primarily presents with symptoms related to vaso-occlusive crises, anemia, and hemolysis. It does not typically involve extensive lymphadenopathy or blast cells in the blood.
-
Question 4 of 10
4. Question
A 68-year-old gentleman, Mr. Smith, on Indapamide for essential hypertension, presents to the emergency department (ED) with vague palpitations and chest pain. His ECG shows T-wave inversion in the inferior leads (II, III, and aVF). Which of the following does not cause T-wave inversion?
Correct
Hyperkalemia is a condition in which the potassium level in the blood is too high. This can cause a number of ECG changes, including peaked T waves, widened QRS complexes, and decreased P waves. However, it does not cause T-wave inversion.
Incorrect answers:
- LBBB is a condition in which the electrical impulse from the heart’s left ventricle is delayed, causing a widened QRS complex. This can also cause T-wave inversion, especially in the inferior leads.
- LVH is a condition in which the left ventricle of the heart is enlarged. This can also cause T-wave inversion, especially in the lateral leads.
- MI is a heart attack that occurs when a coronary artery becomes blocked, preventing blood from flowing to the heart muscle. This can cause T-wave inversion, especially in the leads that correspond to the area of the heart that is affected by the MI.
- Myocardial ischemia is a condition in which the heart muscle is not getting enough blood flow. This can cause T-wave inversion, especially in the leads that correspond to the area of the heart that is affected by the ischemia.
Incorrect
Hyperkalemia is a condition in which the potassium level in the blood is too high. This can cause a number of ECG changes, including peaked T waves, widened QRS complexes, and decreased P waves. However, it does not cause T-wave inversion.
Incorrect answers:
- LBBB is a condition in which the electrical impulse from the heart’s left ventricle is delayed, causing a widened QRS complex. This can also cause T-wave inversion, especially in the inferior leads.
- LVH is a condition in which the left ventricle of the heart is enlarged. This can also cause T-wave inversion, especially in the lateral leads.
- MI is a heart attack that occurs when a coronary artery becomes blocked, preventing blood from flowing to the heart muscle. This can cause T-wave inversion, especially in the leads that correspond to the area of the heart that is affected by the MI.
- Myocardial ischemia is a condition in which the heart muscle is not getting enough blood flow. This can cause T-wave inversion, especially in the leads that correspond to the area of the heart that is affected by the ischemia.
-
Question 5 of 10
5. Question
A new mother brings her 10-month-old son to your clinic. She reports that her son vomits up his entire feed at least once every day. The vomiting is not projectile but rather the feed returns to the mouth and spills over his top. He is otherwise well in himself, with a normal weight for his age. What is the most likely diagnosis?
Correct
Physiological posseting is common in infants, especially around the age of 10 months. It involves non-projectile, effortless vomiting of small amounts of milk or feed. It is considered a normal part of infant development and usually resolves on its own without medical intervention.
Incorrect Answers:
- Gastro-oesophageal reflux disease: This condition typically presents with more severe symptoms such as frequent projectile vomiting, discomfort, and may lead to failure to thrive. It is less likely in a well-growing infant with the described symptoms.
- Lactose intolerance is rare in infants and would typically present with symptoms like diarrhoea, abdominal cramps, and flatulence rather than just vomiting.
- Pyloric stenosis usually presents with projectile vomiting, dehydration, and failure to gain weight. It is less likely in an otherwise well-nourished 10-month-old.
- Infantile colic is characterized by episodes of excessive crying and fussiness in infants, often in the evening. It does not typically involve vomiting and is not the most likely diagnosis in this case.
Incorrect
Physiological posseting is common in infants, especially around the age of 10 months. It involves non-projectile, effortless vomiting of small amounts of milk or feed. It is considered a normal part of infant development and usually resolves on its own without medical intervention.
Incorrect Answers:
- Gastro-oesophageal reflux disease: This condition typically presents with more severe symptoms such as frequent projectile vomiting, discomfort, and may lead to failure to thrive. It is less likely in a well-growing infant with the described symptoms.
- Lactose intolerance is rare in infants and would typically present with symptoms like diarrhoea, abdominal cramps, and flatulence rather than just vomiting.
- Pyloric stenosis usually presents with projectile vomiting, dehydration, and failure to gain weight. It is less likely in an otherwise well-nourished 10-month-old.
- Infantile colic is characterized by episodes of excessive crying and fussiness in infants, often in the evening. It does not typically involve vomiting and is not the most likely diagnosis in this case.
-
Question 6 of 10
6. Question
A 42-year-old woman has recently undergone blood tests, which reveal hypochromic microcytic anaemia, a decreased ferritin level, and a raised total iron-binding capacity. Which of the following is the best treatment for this anaemia?
Correct
This clinical scenario is related to haematology and specifically to the diagnosis and treatment of hypochromic microcytic anaemia, which is often indicative of iron deficiency anaemia. In this case, the patient has a decreased ferritin level, suggesting low iron stores, and a raised total iron-binding capacity, which is a further indicator of iron deficiency. The best treatment for iron deficiency anaemia is iron supplementation, as it replenishes the body’s iron stores, leading to an improvement in the anaemia.
Incorrect Answers:
- Regular transfusion – This is not the first-line treatment for iron deficiency anaemia. Transfusion is typically reserved for severe cases or when other treatments have failed.
- Regular venesection – Venesection involves removing blood from the patient and is not appropriate for treating iron deficiency anaemia.
- Erythropoietin – Erythropoietin is used in conditions where the body is not producing enough red blood cells, but it is not the primary treatment for iron deficiency anaemia.
- Iron chelators – Iron chelators are used to remove excess iron from the body, typically in conditions of iron overload like hemochromatosis, and are not indicated for treating iron deficiency anaemia.
Incorrect
This clinical scenario is related to haematology and specifically to the diagnosis and treatment of hypochromic microcytic anaemia, which is often indicative of iron deficiency anaemia. In this case, the patient has a decreased ferritin level, suggesting low iron stores, and a raised total iron-binding capacity, which is a further indicator of iron deficiency. The best treatment for iron deficiency anaemia is iron supplementation, as it replenishes the body’s iron stores, leading to an improvement in the anaemia.
Incorrect Answers:
- Regular transfusion – This is not the first-line treatment for iron deficiency anaemia. Transfusion is typically reserved for severe cases or when other treatments have failed.
- Regular venesection – Venesection involves removing blood from the patient and is not appropriate for treating iron deficiency anaemia.
- Erythropoietin – Erythropoietin is used in conditions where the body is not producing enough red blood cells, but it is not the primary treatment for iron deficiency anaemia.
- Iron chelators – Iron chelators are used to remove excess iron from the body, typically in conditions of iron overload like hemochromatosis, and are not indicated for treating iron deficiency anaemia.
-
Question 7 of 10
7. Question
A 45-year-old female patient named Sarah presents with a history of systemic sclerosis and signs of renal involvement. She also has a past medical history of lupus nephritis. Her recent lab results indicate elevated serum creatinine levels and proteinuria.
Considering her medical history and current condition, which of the following circumstances should angiotensin-converting enzyme (ACE) inhibitors be avoided where possible?
Correct
Glomerulonephritis and lupus nephritis are both autoimmune in origin and aside from supportive measures and renoprotection with drugs including ACE inhibitors, immunosuppression is commonly used and works with varying effect.
Systemic sclerosis can affect the afferent arterioles with fibrinoid thickening and vessel narrowing, which can come on rapidly (scleroderma renal crisis).
Immunosuppression is often unhelpful, whereas ACE inhibitors are of immense benefit and can halt progression of loss of renal function and sometimes even partially reverse it. In severe renal artery stenosis, ACE inhibitors can further reduce or abolish glomerular filtration. This is because angiotensin normally increases glomerular capillary perfusion pressure, and so when ACE inhibitors reduce this ability, with a background of already grossly reduced renal perfusion, the glomerular filtration rate will fall.
For this reason, the response to ACE inhibitors should be monitored in patients with renal failure (and especially so in patients with known peripheral arterial disease), and if renal function worsens, various imaging techniques can be used to look for renal artery stenosis (such as Doppler ultrasound and renal arteriography).
Overall, whilst ACE inhibitors should be avoided where possible in patients with renal artery stenosis, they are beneficial in protecting the kidneys of renal failure patients, and under specialist supervision can be started at a reduced dose in patients with renal artery stenosis, especially if there is hypertension that cannot be controlled by other means.
Incorrect
Glomerulonephritis and lupus nephritis are both autoimmune in origin and aside from supportive measures and renoprotection with drugs including ACE inhibitors, immunosuppression is commonly used and works with varying effect.
Systemic sclerosis can affect the afferent arterioles with fibrinoid thickening and vessel narrowing, which can come on rapidly (scleroderma renal crisis).
Immunosuppression is often unhelpful, whereas ACE inhibitors are of immense benefit and can halt progression of loss of renal function and sometimes even partially reverse it. In severe renal artery stenosis, ACE inhibitors can further reduce or abolish glomerular filtration. This is because angiotensin normally increases glomerular capillary perfusion pressure, and so when ACE inhibitors reduce this ability, with a background of already grossly reduced renal perfusion, the glomerular filtration rate will fall.
For this reason, the response to ACE inhibitors should be monitored in patients with renal failure (and especially so in patients with known peripheral arterial disease), and if renal function worsens, various imaging techniques can be used to look for renal artery stenosis (such as Doppler ultrasound and renal arteriography).
Overall, whilst ACE inhibitors should be avoided where possible in patients with renal artery stenosis, they are beneficial in protecting the kidneys of renal failure patients, and under specialist supervision can be started at a reduced dose in patients with renal artery stenosis, especially if there is hypertension that cannot be controlled by other means.
-
Question 8 of 10
8. Question
A 65-year-old woman presented with a lesion on her forearm for 4 months. On examination, the lesion is 8 mm in diameter and is a flat, mildly erythematous patch with a few scales and a larger keratotic horn in the center. There are no other lesions on inspection of her skin, and no personal or family history of skin cancer. Which of the following is the most appropriate management plan?
Correct
The most appropriate management plan in this case is Cryotherapy. Cryotherapy involves freezing the lesion with liquid nitrogen, which is effective for treating actinic keratoses, which often present as scaly patches with a keratotic horn. It is a minimally invasive procedure and suitable for isolated lesions without the need for wide excision or biopsy.
Incorrect Answers:
- Wide local excision is generally reserved for larger or invasive skin lesions and may be an excessive approach for this case.
- Topical 5-fluorouracil is commonly used for actinic keratoses but may not be the first choice for a lesion with a larger keratotic horn.
- Excisional biopsy is performed when malignancy is suspected, and this lesion does not present with clear signs of malignancy.
- Curettage involves scraping the lesion, but cryotherapy is a more suitable option for this presentation.
Incorrect
The most appropriate management plan in this case is Cryotherapy. Cryotherapy involves freezing the lesion with liquid nitrogen, which is effective for treating actinic keratoses, which often present as scaly patches with a keratotic horn. It is a minimally invasive procedure and suitable for isolated lesions without the need for wide excision or biopsy.
Incorrect Answers:
- Wide local excision is generally reserved for larger or invasive skin lesions and may be an excessive approach for this case.
- Topical 5-fluorouracil is commonly used for actinic keratoses but may not be the first choice for a lesion with a larger keratotic horn.
- Excisional biopsy is performed when malignancy is suspected, and this lesion does not present with clear signs of malignancy.
- Curettage involves scraping the lesion, but cryotherapy is a more suitable option for this presentation.
-
Question 9 of 10
9. Question
A 60-year-old man presents to his GP with a 4-month history of daily dizzy spells. These last a few minutes and occur when he moves his head. The attacks are not associated with any deafness or tinnitus. Both ENT and neurological examinations are normal. You favour a diagnosis of benign paroxysmal positional vertigo (BPPV).
Which of the following descriptions of findings on Hallpike’s manoeuvre would confirm this diagnosis?
Correct
Benign paroxysmal positional vertigo (BPPV) is caused by debris blocking the normal flow of endolymph in the labyrinth, leading to misreporting of positional change by the vestibules, and a discrepancy between actual position and the position of the head according to the vestibules.
Thus, nystagmus occurs as two different inputs compete for different oculomotor outputs, and vertigo (the perception that the world is moving) ensues. This happens only when the head moves and there is no vertigo with a still head. It usually affects one side only, and thus Hallpike’s manoeuvre (below) only reveals nystagmus when the patient’s head is tilted back whilst they face one side and not the other.
Torsional nystagmus is normally seen after a few seconds of the head being tilted back – it is important to keep the patient lying back for some time. The nystagmus should wear off after around 20 seconds, and on repeat testing it lasts a shorter amount of time (“fatiguing”).
This is the basis of vestibular exercises, which are designed so that compensatory mechanisms may be induced more swiftly and the vertigo attacks will thus become less frequent and less disabling.
Incorrect
Benign paroxysmal positional vertigo (BPPV) is caused by debris blocking the normal flow of endolymph in the labyrinth, leading to misreporting of positional change by the vestibules, and a discrepancy between actual position and the position of the head according to the vestibules.
Thus, nystagmus occurs as two different inputs compete for different oculomotor outputs, and vertigo (the perception that the world is moving) ensues. This happens only when the head moves and there is no vertigo with a still head. It usually affects one side only, and thus Hallpike’s manoeuvre (below) only reveals nystagmus when the patient’s head is tilted back whilst they face one side and not the other.
Torsional nystagmus is normally seen after a few seconds of the head being tilted back – it is important to keep the patient lying back for some time. The nystagmus should wear off after around 20 seconds, and on repeat testing it lasts a shorter amount of time (“fatiguing”).
This is the basis of vestibular exercises, which are designed so that compensatory mechanisms may be induced more swiftly and the vertigo attacks will thus become less frequent and less disabling.
-
Question 10 of 10
10. Question
A 40-year-old woman, Ms. Jones, presents to her primary care physician (PCP) with a 5-week history of unintentional weight loss of 6 kg. She reports that her appetite has been normal and she has not made any changes to her diet or exercise routine. She also complains of fatigue, irritability, and blurring of her vision. On physical examination, her pupils are dilated and she has a “staring look” with lid lag and lid retraction. What is the most likely diagnosis?
Correct
Graves’ disease is an autoimmune disorder that causes the production of excessive amounts of thyroid hormone. This can lead to a number of symptoms, including weight loss, fatigue, irritability, and blurred vision. The physical examination findings of lid lag and lid retraction are also consistent with Graves’ disease.
Incorrect answers:
- Hashimoto thyroiditis is an autoimmune disorder that causes the destruction of the thyroid gland. This can lead to hypothyroidism, which is characterized by weight gain, fatigue, and cold intolerance.
- Multinodular goiter is a noncancerous enlargement of the thyroid gland. It is usually not associated with any symptoms.
- Myasthenia gravis is a neuromuscular disorder that causes muscle weakness. It is not associated with weight loss, fatigue, or blurred vision.
- Toxic thyroid adenoma is a benign tumor of the thyroid gland that produces excessive amounts of thyroid hormone. It is similar to Graves’ disease in its presentation, but it is less common.
Incorrect
Graves’ disease is an autoimmune disorder that causes the production of excessive amounts of thyroid hormone. This can lead to a number of symptoms, including weight loss, fatigue, irritability, and blurred vision. The physical examination findings of lid lag and lid retraction are also consistent with Graves’ disease.
Incorrect answers:
- Hashimoto thyroiditis is an autoimmune disorder that causes the destruction of the thyroid gland. This can lead to hypothyroidism, which is characterized by weight gain, fatigue, and cold intolerance.
- Multinodular goiter is a noncancerous enlargement of the thyroid gland. It is usually not associated with any symptoms.
- Myasthenia gravis is a neuromuscular disorder that causes muscle weakness. It is not associated with weight loss, fatigue, or blurred vision.
- Toxic thyroid adenoma is a benign tumor of the thyroid gland that produces excessive amounts of thyroid hormone. It is similar to Graves’ disease in its presentation, but it is less common.
Based on the MLA Content Map
UKMLA AKT QBank
4000+ revision questions is aligned with the GMC MLA Content Map, assuring you that our QBank is tailored to the AKT exam content.